INTRODUCTION
Medical problems can cause overgrooming or alopecia, including feline cystitis, auto-immune or internal diseases and cancers, (Waisglass et al., 2006), so start with your vet. There is very often a medical reason for overgrooming rather than mere stress or psychogenic alopecia (Waisglass et al., 2006). You may need to find a specialist vet. Flea allergy is a common cause, and other parasite possibilities include include lice or fungal infections. Diagnosis involves ruling out various possibilities (Moriello 2005). A diagnosis cannot be made purely from the area of hair loss (Hobi et al., 2011). Cats can be affected by multiple allergies or a mixture of more than one cause (Landsberg 2009). A survey of cats that had been diagnosed with ‘compulsive’ overgrooming, revealed that most of them had an underlying medical/veterinary cause for their behaviour (Waisglass et al., 2006). Here are the main causes.

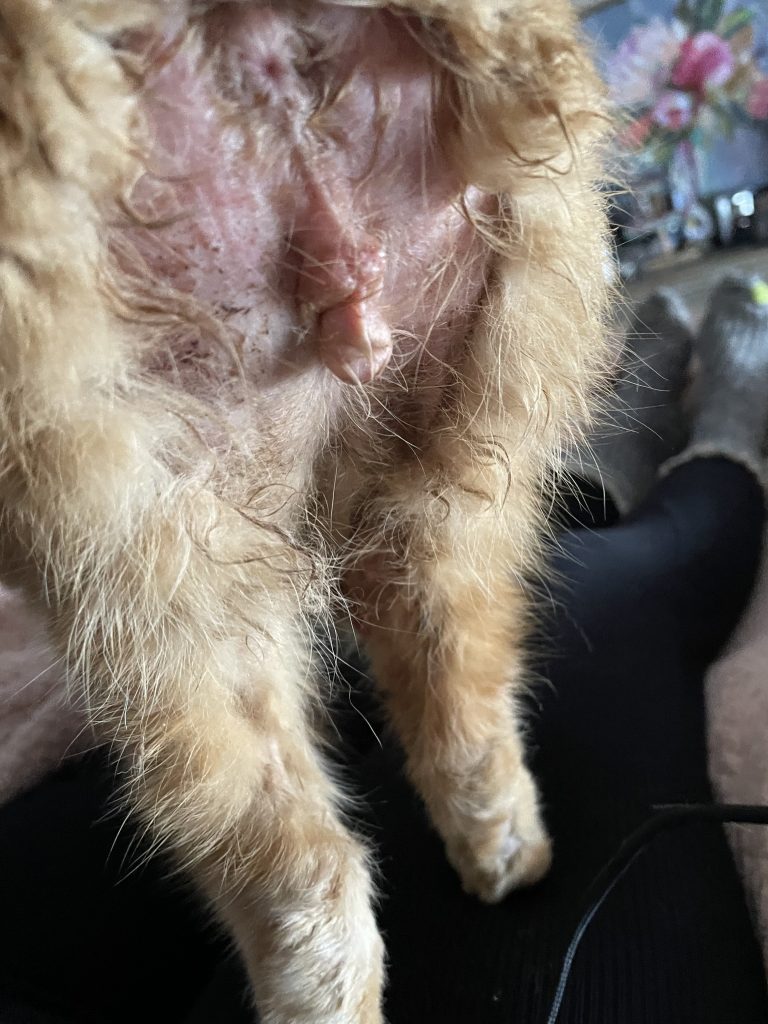
Overgrooming due to ringworm showing that a proper vet work up is essential Article here
SYMPTOMS
The hallmark of the allergy is itchiness, although some cats rarely scratch or lick in front of their owners. Furballs or hairs around the tongue, teeth or house may be signs of excessive licking. Some cats will appear to go bald, although the hairs are really being broken off by licking. Fleas can cause small crusts along the back (called miliary dermatitis) whereas crusting and ulcers around the head and neck may suggest food allergies or ear mites. Some cats develop large red, moist and weeping sores (called eosinophilic plaques), on the belly and leg. However, a diagnosis cannot be made merely on where the overgrooming is evident.
FIRST LINE DIAGNOSIS
Your vet will want to rule out lice and mites, ringworm and treat any infections before investigating allergic diseases. Vets also need to rule out diseases (Landsberg 2009), pain (Caney 2007) or cystitis (Gunn-Moore 2003). Pain will require treatment.
REFERRAL
Just as in human medicine, there are general and specialist vets. There are a number of veterinary dermatologists throughout the UK. Referral appointments can only be made through your own vet, who may suggest a referral, or you can ask them to make an appointment for a specialist opinion.
1. FLEA ALLERGY
This is the most common allergy (O’Dair 1992). Rigorous flea control should be the first step, irrespective of whether fleas can be found. It only takes one flea bite to set off a reaction in allergic cats. The best products to use on your cat are long-acting sprays and spot-on remedies prescribed by your vet. Over-the-counter flea products are not as effective as vet prescribed treatments. A simple flea comb is also worth using regularly to make sure the fleas really have gone. You will also need to treat the surroundings, every room the cat uses, with a safe flea spray. Get vet advice on this and follow the instructions to keep your cat safe. counter products are relatively less effective. Ultrasonic collars don’t kill fleas (Hinkle et al.,1990) and may upset your cat with their sound (Roe & Sales, 1992). Eggs and larvae in carpets and furnishings should also be treated. Sprays with an insecticide and growth inhibitor, are most effective for the environment. There is also another product which is available as a pill. All these products are available from your vet. Flea control trials usually last for 4-5 weeks. Remember to treat all the dogs and cats in the house and continue indefinitely; stop treatment and the fleas will return. Beware – over the counter flea products sold for dogs only may kill cats.
2. FOOD ALLERGIES
The next step is to investigate food allergy. Among cats with skin disorders, somewhere between 12- 17% may be suffering from a food allergy (Bryan & Frank 2010). Other surveys give a higher proportion of food allergy cases (Waisglass et al., 2006). Food allergy tests are not reliable (Mueller & Olivry 2017). Special veterinary diets, for a food trial, are available from your vet. These need either to be a exclusion diets (ingredients cats have never ever eaten before) or be hydrolised protein and good ones in the UK include Hills ZD (wet or dry) and Purina HA. Read Food Intolerance in Cats on this website. Over the counter cat-foods contain a variety of ingredients that vary from batch to batch and are not suitable (Bryan & Frank 2010), even the ones labelled “hypoallergenic”. Trial diets should be fed for at least eight weeks, though an improvement may be seen earlier. Cats should not be fed anything else during the trial. Cats that hunt or are fed elsewhere may need to be kept indoors.
Allergic diseases will wax and wane, so an improvement does not absolutely definitely mean the cat has food allergy. A relapse within 1-2 weeks on the original diet confirms a food allergy. Once stable again on the trial diet, introduce ingredients such as beef, lamb, dairy products etc. one at a time to discover which the cat reacts to. These can then be avoided.
Alternatively, a special diet can be used long term (Leistra & Willemse, 2002). This is often the easiest option.
3. ATOPY OR ATOPIC DERMATITIS
If skin problems persist then allergy tests can be used to identify what your cat is allergic to – the allergens – for treatment or avoidance. Allergy tests should be carried out by an experienced veterinary dermatologist. The effectiveness of these tests is controversial (Bryan & Frank 2010).
a) Skin testing. Cats are sedated and the fur on the side of the chest clipped. Several dust mite, insect, pollen and mould extracts are injected and any reactions noted. Most reactions occur within 20 minutes although some may take 12-24 hours. Skin tests are very specific, but some cats have negative tests.
b) Serological tests. A blood sample is taken and sent off for laboratory testing. The tests show which allergens are producing antibodies in the blood. Serological tests are not quite as exact as skin tests, and are not necessarily cheaper. They are useful if skin tests fail, or if the cat’s skin is in such bad condition that a skin test cannot be run.
TREATMENTS
1. Basic Treatment
Thorough flea control is important in all cases of allergic skin disease. Regular worming and a high quality balanced diet will also be of benefit.
2. Lifestyle Management
Some allergens can be avoided. Dust mites and pollens are ubiquitous, but keeping cats out of bedrooms and carpeted rooms, using solid or washable cat-beds, vacuum cleaners with filters and improving ventilation will help.
3. Immunotherapy
Most veterinary dermatologists use immunotherapy to desensitise your cat by giving regular injections of allergens identified by skin or blood tests. Most cats tolerate the injections very well. Your vet will usually administer the first few injections in the unlikely chance of an allergic shock, or anaphylactic, reaction, but most owners give the injections at home thereafter. Mild itching and injection site nodules are minor problems. Many, but not all, cases respond to immunotherapy.
4. Anti-inflammatory Treatment
Anti-inflammatory treatment may be necessary if your cat does not respond to immunotherapy. Short-term treatment may be used during flea control or food trials.
a) Antihistamines
Many of these drugs are available from pharmacists, but the doses in cats are different from people, and they should only used under veterinary supervision. Your vet will try 3-4 drugs to select the most effective. Side effects are uncommon, but include sedation and vomiting. Only about 50% of cats respond to antihistamines, although the response may improve if they are combined with essential fatty acids.
b) Essential Fatty Acids
These are fish and plant (e.g. Evening Primrose or Borage) oils. Veterinary products are preferred unlike cheaper brands that vary from batch to batch. The initial course is usually eight weeks, although again no more than 50% of cases respond.
c) Steroids
These are cheap and effective, but can have serious side effects (including weight gain, excessive drinking and urinating, infections, diabetes, liver and skin problems) and are generally used as a last resort. Many cats tolerate low doses of steroids given on alternate days quite well. Using other treatments often reduces the dose required. Cats on long-term steroids should have regular check ups.
5. Other Treatment Options
Without controlled studies it is difficult to know if alternative remedies are of any benefit. Many human remedies can be quite toxic in cats and should only be given under veterinary supervision. Female sex hormones (e.g. Ovarid®) have little role in feline dermatology. Serious side effects are common, and these drugs should only be used to treat specific conditions by an experienced veterinary dermatologist. Any alternative remedies should be passed by the vet before being used.
4. STRESS
Fur pulling can be a response to stress. It may start off for a different reason, such as pain, then continue as a habit. The longer it goes on, the more difficult it is to stop. Read Reasons Why Your Cat is Stressed on this website and take remedial action.
An itchy cat is an unhappy cat and making sure it has the best environment will help it recover even if the cause is not primarily stress but is also medical (Landsberg 2009). Occasionally some cats may start to use overgrooming as an attention seeking device. Punishing, rebuking or picking up the cat may give the cat the attention it seeks, making overgrooming more likely to occur (Virga 2003).
A cat behaviour counsellor will help you discover what is bugging your cat. It’s difficult for owners to see what is wrong.
There is an interesting vet talk about overgrooming here.
REFERENCES
Bryan, J., & Frank, L., (2010) ‘Food allergy in the cat. A diagnosis by elimination,’ Journal of Feline Medicine and Surgery, 12, 861-866.
Caney, S., ‘Feline Arthritis’, Veterinary Focus, 17, (3), 11-17
Gunn-Moore, D. A. (2003), ‘Feline lower urinary tract disease,’ Journal of Feline Medicine and Surgery, 5, 133-138.
Hinkle, N. C., Koehler, P. G. & Patterson, R. S., (1990), ‘Egg Production, Larval Development, and Adult Longevity of Cat Fleas (Siphonaptera: Pulicidae) Exposed to Ultrasound,’ Journal of Economic Entomology, 83, 2306-2309
Hobi, S., Linek, M.,Marignac, M., Olivry, T., Beco, L., Nett, C., Fontain, J., Roosje, P., Bergvall, K., Belova, S., Koebrich, S., Pinn, D., Kovalik, M., Meury, S., Wilhelm, S. & Favrot, C., (2011), ‘Clinical characteristics and causes of pruritus in cats: a multicentre study on feline hypersensitivity- associated dermatoses,’ Veterinary Dermatology, 22, 406-413.
Landsberg, G., (2009), ‘Self trauma in dogs and cats. Is it medical or is it behavioral?’. Accessed at http://veterinarycalendar.dvm360.com/avhc/content/printContentPopup.jsp?id=650428 Downloaded August 9 2012.
Leistra, M., & Willemse, T., (2002), ‘Double blind evaluation of two hypoallergenic diets in cats with adverse food reactions,’ Journal of Feline Medicine and Surgery, 4, 185-188.
Moriello, K., (2005), ‘Self mutilation and Overgrooming in a Siamese Cat’, Veterinary Medicine,
Mueller, R.S. & Olivry, T., (2017), ‘Critically appraised topic on adverse food reactions of companion animals (4): can we diagnose adverse food reactions in dogs and cats with in vivo or in vitro tests?’ BMC Vet Res.;13(1):275.
O’Dair, H., (1992), ‘Differential Diagnosis of Pruritus,’ In Practice, 14, 185-192.
Roe, D.J. Sales, G. D., (1992), ‘Welfare implications of ultrasonic flea collars,’ The Veterinary Record, 130, 142-143,
Tanglinger, K., Helps, C. R., Day, M. J. & Foster A. P., (2005), ‘Measurement of serum immunoglobulin E (IgE) specific for house dust mite antigens in normal cats and cats with allergic skin disease, ‘ Veterinary immunology and immunopathology, 105., 85-93.
Virga, V., (2003), ‘Behavioral Dermatology,’ Clinical Techniques in Small Animal Practice, 33, 231-251.
Waisglass, S. E., Landsberg, G. M., Yager, J. A. & Hall, J. A., (2006), ‘Underlying medical conditions in cats with presumptive psychogenic alopeci’, JAVMA, 228, 1705-1709.
Willemse, T., & Spruijt B. M., (1995), ‘Preliminary evidence for dopaminergic involvement in stress-induced excessive grooming in cats,’ Neuroscience Research Communications, 17, 203-208
Willemse, T., (2009), ‘Feline Atopic Dermatitis – Sense or Nonsense?’, Proceedings of the Southern European Veterinary Conference & Congreso Nacional AVEPA 2009,
Wolberg, A. C. & Blanco, A., (2008) ‘Pruritis in the cat’, Veterinary Focus, 18, 4-11